UBT Consultants & UPRs
Help Video
How to Find UBT Basics on the LMP Website
LMP Website Overview
How to Find How-To Guides
This short animated video explains how to find and use our powerful how-to guides
How to Find and Use Team-Tested Practices
Does your team want to improve service? Or clinical quality? If you don't know where to start, check out the team-tested practices on the LMP website. This short video shows you how.
How to Use the Search Function on the LMP Website
Having trouble using the search function? Check out this short video to help you search like a pro!
How to Find the Tools on the LMP Website
Need to find a checklist, template or puzzle? Don't know where to start? Check out this short video to find the tools you need on the LMP website with just a few clicks.
Team Member Engagement
When UBT members are actively involved with their team, they speak up with their best ideas about how to improve the department. They take advantage of partnership processes like consensus decision-making and interest-based problem solving to make the department a great place to work. They look at how the department is doing on key metrics—like those around service and quality—and use that information to come up with ideas for improvement.
Deck: The following report helps to illustrate how the KP model delivers quality and affordability
Health care costs too much. The cost of care threatens Kaiser Permanente’s social mission to provide affordable, quality health care to all.
There are no simple solutions, but KP has many advantages that others do not—including our integrated model of care that can better manage and prevent illness; a prepaid, nonprofit structure that keeps revenue in the system to better serve members and patients; and unit-based teams. As they create the best place to work, UBTs are continuously improving quality, service and affordability at the front lines of care.
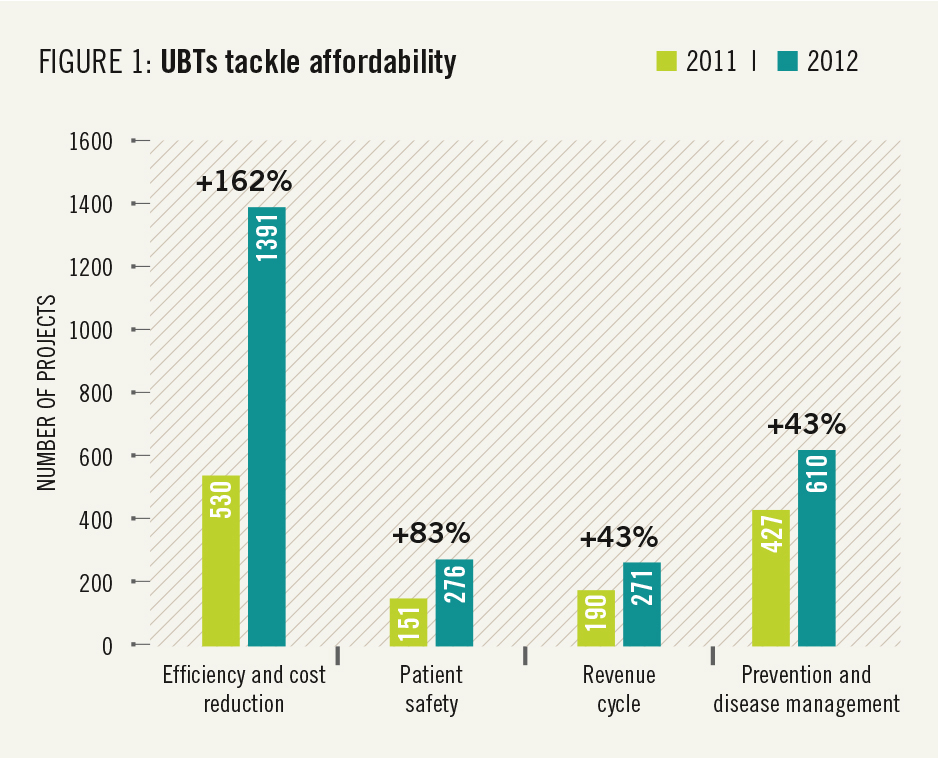 This report highlights many ways that unit-based teams are getting results that matter to members and patients. Affordability of care, one of the issues that matters most to members, was the fastest-growing focus area for UBTs in 2012 (see Figure 1).
This report highlights many ways that unit-based teams are getting results that matter to members and patients. Affordability of care, one of the issues that matters most to members, was the fastest-growing focus area for UBTs in 2012 (see Figure 1).
Teams launched nearly 1,400 efficiency and cost-reduction projects last year, more than doubling the number of such projects undertaken in 2011.
That bodes well for the future, because the number and effectiveness of UBTs’ performance improvement projects increase as teams develop. For instance, UBTs that are rated high performing—defined as reaching Level 4 or 5 on the UBT Path to Performance—are three times more likely than Level 1 teams to take on cost-reduction projects, using proven tools such as process mapping, the “6S” performance improvement tool, and spaghetti diagrams (see Figure 2).
 And these teams are getting results. Waste- and cost-reduction projects can yield immediate savings of $20,000 to $50,000. Spread across the organizations, these efforts could save more than $100 milliion a year. Some examples of the work being done:
And these teams are getting results. Waste- and cost-reduction projects can yield immediate savings of $20,000 to $50,000. Spread across the organizations, these efforts could save more than $100 milliion a year. Some examples of the work being done:
- At the Baldwin Park Medical Center Laboratory in Southern California, phlebotomists worked to reduce the use of more expensive butterfly needles, substituting standard needles when they will work—saving more than $45,000 in 2012. Other labs are also doing this; potential savings if implemented program-wide: $2 million.
- The Fremont Medical Center Operating Room team in Northern California, after taking business literacy training and looking at their own costs and budget, identified wasteful practices in the use of ready-made surgical supply packs, saving about $34,000 a year. Potential savings if implemented program-wide: $750,000.
- The Point Loma Primary Care team at the San Diego Medical Center in Southern California applied 6S to organize supplies and standardize ordering, saving more than $20,000 in 2012. Potential savings if implemented program-wide: $4.2 million.
As these examples show, individual teams can implement improvements that can save a significant amount of money in their own corner of the system. As practices spread among the 3,500 unit-based teams now working across Kaiser Permanente, the savings can add up quickly.
Achieving the full cost-saving potential of UBTs will not be automatic. More teams need to take on cost and waste issues. Even with the jump last year, only one-fifth of UBTs undertook such projects. Successful practices must be spread more systematically across departments, facilities and regions. And more teams need the kind of business training that led the Fremont OR team to act.
 But those changes are coming. “The growing number of cost saving and efficiency projects are helping build a culture of savings and waste reduction among high-performing teams across KP,” says Peter Nixon, director of metrics and analytics, Office of Labor Management Partnership.
But those changes are coming. “The growing number of cost saving and efficiency projects are helping build a culture of savings and waste reduction among high-performing teams across KP,” says Peter Nixon, director of metrics and analytics, Office of Labor Management Partnership.
High-performing UBTs outscored others on two questions in the 2012 People Pulse survey regarding employee views of their department’s efficiency. (see Figure 3). Members of high-performing teams are more likely to say their departments have efficient work procedures and seek improvements to reduce costs.
“These findings suggest that members of high-performing teams see waste reduction and efficient work processes as part of their job,” Nixon says. “That is good news, because it’s the discretionary effort, commitment and intelligence of frontline teams that gets results.”
Helping Teams Understand Their Value
Deck: Peer advice from a union partnership representative
As a union partnership representative (UPR) from UFCW Local 770, Annamarie Marin helps support 72 unit-based teams at the West Los Angeles Medical Center. Last year, she helped the Oncology team overcome low morale to move from Level 2 to Level 4—and it’s now on the cusp of achieving Level 5. Marin recently was interviewed about her role as a UPR by LMP Communications Manager Sherry Crosby.
Q. What experiences helped prepare you for your position?
A. I have been part of UBTs since 2005. I started as a co-lead and then became an executive sponsor. This experience helped me tremendously, because I can relate to the teams on a personal level. I have been in the exact same place, dealing with similar challenges.
Q. What is your approach to working with teams?
A. Some teams need team-building exercises, while others need to learn to trust one another and share information on projects. Starter teams don’t know how to create agendas or structure meetings, so I help facilitate their meetings. The most important thing is making sure I’m available and that teams have what they need to succeed.
Q. What early challenges did the Oncology team face?
A. They were struggling with membership involvement and morale was low. Nobody wanted to participate in meetings.
Q. How did you help the team succeed?
A. I helped staff members understand that the UBT is not there to add work to their plate. Eventually, we got a group to participate in team meetings.
We went through different trainings and started on small projects. First, they focused on staff morale. Staff members practiced expressing appreciation for each other until it became part of the team's culture. Then they moved to an affordability project. That was a pivotal point in that team’s development, because the idea came from a labor partner.
It shows team members are involved in decision making and contributing to the department’s success.
Q. What was key to the team’s success?
A. I helped the team members understand their work through a different lens—what the function of a UBT is, and their role in it. They realized they have a great department and an engaged manager. It was really about helping them understand their value to each other.
TOOLS
What Are UBT Health and Safety Champions?
Format:
PDF
Size:
8.5" x 11"
Intended audience:
UBT health and safety champions and those who will recruit volunteers for this role (such as regional co-leads, UBT consultants, union partnership representatives and UBT co-leads)
Best used:
This poster describes the duties of UBT health and safety champions. Post it on bulletin boards, in break rooms or email it to potential UBT health and safety champions.
The Difference Diversity Makes
Deck: How UBTs improve care for our members and patients
For the past few years, unit-based teams have been driving a powerful transformation. It’s helping to control chronic diseases; assisting in the early detection of cancer; providing familiarity with a patient’s community; and enabling frontline employees to speak a patient’s language. It creates customized care for each of Kaiser Permanente’s more than 10 million members.
It isn’t a cool new gadget or something out of a sci-fi flick creating the change, but rather a modern care approach that takes into account the infinite number of ways KP members are unique—that emphasizes diversity and inclusion.
“All of us as individuals have all these different multicultural identities, and so do our patients,” says Ron Copeland, MD, senior vice president of National Diversity and Inclusion Strategy and Policy and chief diversity and inclusion officer. “We have to create high-performing teams that work together to deliver culturally responsive care that addresses those differences.”
Increasingly, the workers, managers and physicians working together in UBTs are considering the many facets of individual patients as they transform—in small and large ways—how they care for and serve those patients, using their knowledge and empathy to rethink how we deliver care.
As the stories in this issue of Hank illustrate, some of those changes are aimed at eliminating race- and gender-based health disparities. Other changes are taking place outside our medical facilities—working with school-age children, for example, to give them better food choices and teach them healthy habits that can last a lifetime.
By doing this, UBT members are ensuring that Kaiser Permanente members are the healthiest they can be no matter their background or beliefs, language or gender, disability or economic status, whether they live in a big city or on a farm.
“UBTs have always led on innovating care by putting patients at the center, listening to them and customizing care for them,” says Hal Ruddick, executive director of the Coalition of Kaiser Permanente Unions. “This work strengthens and deepens that high-quality care.” KP’s workforce is full of diversity, and UBTs are designed to draw on all employees’ perspectives in deciding how best to do the unit’s work. It’s a natural step to include our members’ and patients’ viewpoints as well. Understanding and considering the complexity of the patients and communities we serve directly affects quality of care and health outcomes.
“It’s about using our knowledge of differences as an advantage to better understand the patients we care for,” says Dr. Copeland. “Our goal is health care equity—so that all our patients achieve optimal health. For that to happen, it’s essential that we have approaches that account for our patients’ unique needs, preferences and living conditions.”
Deck: Unit-based teams, already the engine of performance improvement, are set to step it up again
Each day, every day, Kaiser Permanente’s 3,500 unit-based teams are providing ever-better patient care and advancing our mission. Now, under the 2015 National Agreement, UBTs will have an even greater role to play—and higher expectations to meet.
The new contract, which took effect Oct. 1, 2015, calls for UBTs to bring the voice of KP members and patients into their work. Teams also will be making total health and safety a greater part of their activities. And they will undergo more rigorous, face-to-face performance assessments.
To help them meet the new expectations, there’s a cadre of expert peer advisors and coaches they can call on—unit-based team consultants and union partnership representatives (UPRs) trained in performance improvement methods. Both UBT consultants and UPRs support unit-based teams, but UPRs, who are coalition union-represented employees, also specifically mentor and support labor in UBT and performance improvement work. Both help teams sharpen their communication, data collection and analysis, and other skills needed to advance on the Path to Performance.
It’s a unique system to support workplace learning and innovation.
“I’ve learned a lot about how to build teams and how to use performance improvement tools,” says Gage Martin, an SEIU-UHW member and union partnership representative at the Santa Rosa Medical Center in Northern California. “I take that learning and help teams do projects in all areas of our Value Compass. It’s a great job.”
The UBT consultant and UPR roles were created, as a test of change, in 2008. Since then, they have helped KP set the standard for quality, service and the workplace experience, and delivered tens of millions of dollars in cost savings.
As we strive to deliver the promise of One KP—providing each member and patient with the best care experience, every time—we also need to have One LMP, with each person working in partnership, having the same resources available to them and the same accountability to upholding the National Agreement. UBT consultants and UPRs help make that happen.
Deck: UBT consultant looks forward to the day her teams don't need her anymore
When one of her teams is able to leap over the roadblocks in its path with the grace of an Olympic hurdler, Charisse Lewis finds herself out of a job.
As a UBT consultant for the Baldwin Park Medical Center in Southern California, it’s an occupational hazard that she looks forward to—again and again. Like coaches everywhere, she enjoys seeing her teams take what they’ve learned and make it their own.
“I do a lot of mentoring,” says Lewis, who acts as coach, counselor and head cheerleader for her facility’s 68 unit-based teams, nudging them past milestones on the Path to Performance, the five-stage “growth chart” UBTs use to measure success. “I’m teaching teams how to function without me.”
For example, she recently helped a team of critical care nurses advance from Level 1 to Level 4 by using an array of strategies from team-building activities to involving union representatives. Another team advanced to Level 4 in part because she coached the management co-lead, who was new to Kaiser Permanente, in how to manage effectively in a partnership culture.
A team to help teams
Lewis doesn’t work alone. She’s part of Baldwin Park’s UBT Strategy Group, a SWAT team of union members and managers who target at-risk teams. That team’s goal is to help UBTs excel so they can drive performance to provide the best service, quality, affordability and job satisfaction. Low-performing teams, says Lewis, tend to suffer from poor communication, paltry trust and a lack of transparency.
“It’s hard to get past that stuff,” she says. “They flounder there. They don’t trust each other and it’s hard to be a team.”
Part of Lewis’s talent in helping turn teams around is her skill in assessing stumbling blocks and getting teams engaged with the right resources. She draws on her experience as an LMP coordinator, trainer and improvement advisor to nuture her teams.
“I don’t like to stare at that elephant in the room,” says Lewis. “If it’s a contract issue, then we need a contract specialist. If it’s an HR issue, let’s make sure that HR is involved. I like to address the problem and get the team’s leaders involved, from both labor and management.”
Tops in Southern California
Her approach speaks for itself. Baldwin Park has the highest percentage of high-performing teams in Southern California: Of 68 teams at Baldwin Park, 88 percent are at Levels 4 and 5 on the Path to Performance.
Her passion, integrity and ability to help others overcome their differences and work together to improve member and patient care has earned her praise from LMP leaders throughout Southern California—but Lewis, in turn, credits her success to the many people who support her efforts.
“I have the support of the regional LMP office, and I have a strong support system at the medical center,” she says. “It makes my job easier.”
Take action to improve communication
If you are inspired to improve your team’s communication, just like the ones in Baldwin Park did, here are the next steps for you to take:
- Huddle regularly. Watch our video “Huddle Power.”
- Practice asking questions in an open-ended, solution-oriented way. Download our tip sheet.
- Plan a team-building activity or even a fun icebreaker for your next meeting to build trust.
Deck: Improving team culture and paving the way for high performance can require expert assistance
For years, success eluded the Baldwin Park Critical Care team. Mired in distrust, staff members didn’t participate in unit-based team meetings. As recently as 2011, few in the 49-member department knew the team existed.
“I didn’t even know what UBT stood for,” says Sheryl Magpali, RN, a member of UNAC/UHCP and now the team’s union co-lead. “No one claimed to be part of it. It was pretty much nonexistent until 2013.”
With a new manager on board, interest in the UBT grew. Staff members from the Critical Care Unit and its sister department, the Step-Down Unit, elected 12 representatives, who in turn chose Magpali as the labor co-lead. Celso Silla, RN, the new department administrator, became the management co-lead.
Old issues die hard
It was rough going at first.
Attendance was spotty. When the team did meet, members focused on long-simmering grievances about labor and personnel issues. The team reached out to Charisse Lewis, Baldwin Park’s UBT consultant. While consultants often focus on helping teams with using the Rapid Improvement Model and designing tests of change, they also help teams learn to work as teams—clearing up issues that are distracting them from the work at hand.
Lewis’s first steps were to encourage the team’s union members to meet separately with a labor representative.
“That helped relieve the stressors of the union issues,” Magpali says. Now, she says, “team meetings focus on changes that affect the unit, rather than things we have no control over.”
The department—nearly all nurses, but also including ward clerks, who are SEIU-UHW members and one of whom is a team representative—began building trust in other ways, too. At Lewis’s suggestion, staff members organized a bowling night and had dinner together. This summer, they held a backpack drive.
Moving the team forward
“Charisse has been good at guiding us—attending our meetings, observing and listening and seeing how we can do better,” says Silla.
Lewis didn’t stop with team-building activities. She coached Magpali, a soft-spoken nurse, to speak up during meetings and make her voice heard, and she helped Silla overcome his reluctance to leave his union co-lead in charge of meetings.
Once trust was established, the team could turn its attention to improving patient care, with remarkable results. UBT members have reduced central line-associated bloodstream infections from five in 2014 to none as of August of this year. Buoyed by that success, they are working to reduce catheter-associated infections.
Silla attributes the improvements to the culture of partnership and putting frontline employees in charge of decisions that affect their work.
“We would have been in limbo” without Lewis’s guidance, Silla says. “Now we’re on the same page. We can be a Level 5 in the future.”
Deck: Helping teams make sense of their data
When it comes to metrics, even the best teams can get muddled.
At such times, a good team realizes it needs help—that it’s time to ask for assistance from someone with specialized skills. In the Northwest region, teams can turn to Ed Vrooman.
His enviable strength? An ability to crunch numbers, connect the dots and break down the complexity of the data so that unit-based teams get the information they need to do their work.
“It’s easy for teams to fall into analysis paralysis, where they dissect every data point. I work with them to know the why and the what,” says Vrooman, who started as a part-time phlebotomist 18 years ago at Portland’s now-long-gone Bess Kaiser Hospital. Today, he does double duty as a union partnership representative (UPR) for the Coalition of Kaiser Permanente Unions—he’s a member of SEIU Local 49—and as an improvement advisor.
A broad perspective
His atypical career path has given him an unusual outlook. In 2003, Vrooman took an extended leave of absence to work for Local 49, helping organize KP employees and other health care workers. After returning to KP, he became a labor partner and brought the coalition’s interests to the building of the new Westside hospital and other major regional projects.
“Partnership has allowed me to touch nearly every function within this organization,” Vrooman says. Working on the large initiatives got him more intrigued with the data side of the house—and led to his current position, which gives him an opportunity to use his skill with data and analytics.
When he heard from the region’s UBT consultants that teams didn’t have the data they needed to work on projects, Vrooman became—along with the data analytics department and health plan leaders—a driving force in the creation of the region’s scorecards for teams. The STATIT scorecards (named after the electronic system that hosts them) enable teams to see their goals online and how they line up with the regional and PSP goals.
Co-leads’ gathering
Every year, Vrooman, along with the other two UPRs in the region—Bruce Corkum, RN, an OFNHP/ONA member, and Mariah Rouse of UFCW Local 555—present information on regional goals and budgets in one of the quarterly Steward Councils, which bring together the region’s UBT union co-leads and representatives from its four partnership unions. For the meeting on regional goals, the management co-leads are invited as well, providing a chance for team leaders to learn together how their teams can have an impact.
When he’s working directly with a team, Vrooman mentors and coaches its members on using improvement tools, from understanding the fundamentals such as SMART goals and entering projects into UBT Tracker to more advanced tools like process mapping. He asks his team members what they need to be successful.
“You don’t need a title to be a leader,” Vrooman tells them. “You lead from where you stand.”

