Deck: All in a Day's Work

This short animated video explains how to find and use our powerful how-to guides
Does your team want to improve service? Or clinical quality? If you don't know where to start, check out the team-tested practices on the LMP website. This short video shows you how.
Having trouble using the search function? Check out this short video to help you search like a pro!
Need to find a checklist, template or puzzle? Don't know where to start? Check out this short video to find the tools you need on the LMP website with just a few clicks.


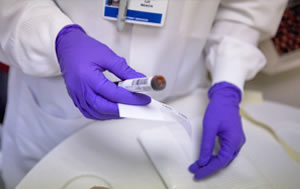
Hemaxi Khalashi isn’t afraid of strange smells. As a clinical lab scientist, her nose is in all kinds of odd odors. But the stench that filled her corner of the Northern California Regional Lab one recent morning put her and many of the other lab workers on edge.
“It was like a bad, old gassy smell, or something deteriorating,” Khalashi said. “I asked my supervisor to walk with me to that corner of the room and asked her what she smelled, and she said, ‘Something dead—rotten.’”
The lab employees quickly fingered the culprit—a new instrument that tests blood samples for Hepatitis B—but they needed a solution, and fast. Their first step: to huddle.
The 15-minute meeting gave lab workers the chance to air their concerns, and provided managers with the opportunity to let the team know the vendor already had been contacted and would be coming by that day. Khalashi spoke up and asked what could be done, right away, to help those who worked near the machine. The section manager suggested masks, which are always available for lab employees.
“Huddles are usually the starting point for getting something done,” said Larry Ratto, a lab assistant and SEIU UHW-West member whose desk is the rallying spot for such meetings. “They are really good for making immediate change—and they never last more than 15 minutes, tops.”
In short order that morning, an issue that might have caused an undercurrent of anxiety was aired and laid to rest. Lab employees and managers determined test results weren’t being compromised and that the odor, though unpleasant, was harmless—and thanks to the huddle, everyone knew it. They later decided to install an air purifier next to the instrument and developed new procedures for handling its waste. The two steps have mitigated the smell.
The lab workers’ instinct to huddle, which stemmed from a year’s worth of practice, is one shared by many high-performing teams throughout Kaiser Permanente. The most successful unit-based teams, those that improve performance and meet goals, are using huddles regularly and effectively—and not just when a major problem needs to be solved.
Huddles aren’t a substitute for the training and skill-building that members of unit-based teams need as they shift into new ways of working—training and skills that help create the learning environment where frontline workers are engaged in decision making and see the connection between their work and larger, strategic outcomes.
But those who study group dynamics say routine huddles can give teams the opportunity to get good at solving problems together when the stakes are low—practice that increases the odds of solving problems successfully when the stakes are high. Frequent, candid conversations, these experts say, create working environments conducive to improvement and change.
“I see it in our group,” said Denise Ja, microbiology section manager. “Huddles have improved our communication, our camaraderie and our teamwork.”
Amy Edmondson, a Harvard Business School professor whose research examines what factors foster outstanding performance in health care settings, says huddles are a way of building what sociologists call “social capital.” In other words, they build social connections that produce real value by increasing productivity.
“The more we know each other and…(have) exchanged our thinking, the more we’ve just connected as human beings—the better we do,” said Edmondson, who led two workshops at this spring’s Union Delegates Conference. “If we’re friends, I will make that extra little cognitive effort to think, ‘Oh, I wonder why she thinks it’s that way?’ Or, ‘I wonder why she sees it that way?’”
The willingness to extend that extra effort can make a world of difference in solving problems, creating a healthy work environment—and improving patient outcomes.
In Northern and Southern California, 79 percent of high-performing UBTs were huddling as of November 2009. Just 30 percent of newly established teams were doing the same. Once a team has gotten trained in the Rapid Improvement Model and other fundamental techniques, huddles can be an addition that helps improve working relationships.
Huddles mean different things to different departments. Some teams meet daily; others do it weekly. Many departments convene at the same time and same place; others are more spontaneous. Most huddles are short.
Part of what makes huddles effective is that they create frequent, regular opportunities for all the members of the unit-based team—the people whose work naturally draws them together—to come together and contribute ideas.
And they have a casualness that makes even the most reticent team member comfortable speaking up.
“I think because we’re close together in physical proximity, people feel less inhibited,” Ja said. She finds that in more formal meetings, some team members hold back. But when the team huddles in the work area, she said, “It’s kind of a hustle-bustle, and people are anxious to put their two cents in.”
Ja’s team usually huddles every Friday. But during the height of the H1N1 epidemic, the number of specimens the lab handled skyrocketed from 30 to 900 per day, and the team resorted to meeting daily and sometimes even hourly.
As team members worked frantically to devise a new system for tracking samples, the huddles became the place to test new ideas. It was in a huddle that someone suggested a coding system using letters, but the team quickly ran through the alphabet. The team members huddled and re-huddled until they were using a combination of letters, dates and numbers.
Huddles helped the lab workers keep up with the onslaught of work, pulling off what had seemed impossible.
“Everyone contributed ideas,” said Mark Stanley, microbiology director. “We depended on everyone’s knowledge.”
Even teams whose members don’t all work in the same location find that huddling works.
Colorado’s asthma care coordinators are spread out across the region, and usually see each other only two or three times a month. But when the department of seven launched a big push to improve the refill rate of an asthma control medication among children, team members decided to huddle once a week over the phone.
During their phone chats, which usually ran 30 to 45 minutes, team members related their progress in reaching out to members ages 5 to 17 who had not refilled their prescription in four months. Developing a habit of sharing their best practices, successes and failures with colleagues made the team members more accountable, said Kristie Wuerker-Delange, RN, an asthma care coordinator and member of UFCW Local 7.
“It’s kind of an, ‘Uh oh, I have to get this done because we’re going to talk to everybody, and they are going to want to know what I’ve been doing for the week,’” she said.
During one huddle, for example, asthma care coordinator Cindy Lamb told the team she had found that promoting the convenience of the mail-order pharmacy, giving members the telephone number to the regular pharmacy, and providing the member’s prescription number helped patients get their refills faster.
Within eight months, the refill rate of inhaled corticosteroids leapt nearly 20 percentage points, from 43 percent in March 2009 to 60 percent in January 2010—a feat that would not have taken longer without their huddles, Wuerker-Delange said.
“They kept the team focused on the same goal,” said Lamb, a member of UFCW Local 7.
While other teams have the benefit of simply moseying over to a colleague’s desk, meeting over the phone has its pluses.
“I feel like people open up a bit more,” Wuerker-Delange said. “They are more apt to say a certain thing if someone’s not looking at them.”
For the Family Medicine department at the Culver Marina Medical Offices campus in Southern California, huddles are part of the morning routine, like brushing your teeth after breakfast.
At 8:25 a.m., Department Administrator Barbara Matthews pokes her head into team members’ offices, her cue that it’s time to convene in the hallway. Patients already are beginning to arrive, so huddles rarely last more than five or 10 minutes.
Doctors, nurses, medical assistants—everyone who is working that day—attend. Co-leads use the time to relay who is working, share a workplace safety message, offer service reminders and more.
“I am upset if I can’t make our morning huddles,” said Krystle Harris, a medical assistant and SEIU UHW-West member. “If I am screening a patient and have to miss it, then I’ll ask one of my co-workers, ‘Aw man, what was the huddle about?’”
Matthews said in the beginning it wasn’t easy getting everyone to huddle and some team members still might choose not to attend if given that option.
But she thinks it’s no coincidence that since the department started huddling a year ago, its hospitality scores have increased, from 83 percent in December 2008 to approximately 89 percent in December 2009.
Other shifts, more subtle but just as significant, are taking place as well. Gene Oppenheim, MD, the physician in charge of the Culver Marina Medical Offices, notes that employees who frequently used to arrive five or 10 minutes late are on time now. Matthews says team members like Harris, who used to say little during meetings, are doing a lot more talking.
That’s a clue that team members are confident their views are valued and they aren’t afraid they may get in trouble for sharing their thoughts—two key characteristics that research shows leads to high performance.
One day recently Harris overheard licensed vocational nurse Jolavette Pye, an SEIU UHW-West member, trying to schedule a specialist appointment for a patient.
The specialist was booked for quite some time, but Pye called back a week later and sure enough, there was a cancellation.
“I brought it to the huddle to congratulate her,” Harris said. “She went out of her way—and the patient was really happy.”
Harris said she thinks sharing with the team the praise she’s overheard co-workers receiving from a patient helps morale, so she does it whenever she can.
“I am shy and I don’t like to speak around a lot of people,” Harris said. “But I am beginning to speak up and discuss little things that are on my mind. I’m just more comfortable in the huddle setting.”
Have questions about huddling you’d like to bounce off one of the team co-leads interviewed for this article? Email Denise.Ja [at] kp.org, Concepcion.Savoy [at] kp.org, Kristine.Wuerker-Delange [at] kp.org, Deana.L.Parker [at] kp.org or Barbara.J.Matthews [at] kp.org for their thoughts.
Here are some tips to help you get the most out of your huddles.
Some ideas of what to discuss:
—From the Sponsor and Leader Resource Guide for UBTs.
Denise Ja, microbiology section manager, Northern California Regional Lab‘Huddles have improved our communication, our camaraderie and our teamwork.’
In high-risk industries—including aviation and high-rise construction as well as health care—surgeon and best-selling author Atul Gawande has found that a good checklist not only specifies common sense safety measures, it also ensures “that people talk to one another about each case, at least just for a minute before starting,” he writes. “[It is] basically a strategy to foster teamwork—a kind of team huddle.”
A major theme of Gawande’s latest book, The Checklist Manifesto: How to Get Things Right, is that the best checklists are not just a top-down set of tasks for others to follow. They’re a tool for better team communication, coordination and inquiry. Read more about using checklists here.
The medical/surgical staff at Fontana Medical Center had a problem with pressure ulcers. The 59-bed unit averaged about 10 of these hospital-acquired bed sores a quarter.
It's painful for the patient and costly for the hospital, which can average about $43,000 per incident. But pressure ulcers are also preventable, and that can lead to shorter hospital stays and improved patient satisfaction scores. Reducing the rate of pressure ulcers can also eliminate inquiries from the California Department of Health Services.
Based on recommendations from the UBT, the staff implemented an education program and provided one-on-one training on how to spot, rate and reduce bed sores.
The team established a strict regimen that included rating patients on the Braden Scale, which helps identify those at risk for pressure ulcers. They performed morning assessments, and used waffle mattresses and moisture-protective barriers for at-risk patients.
They also rounded hourly for turning and got patients out of bed three or four times a day to decrease their risks. This allowed patients to use the restroom and to keep them clean.
“It’s pretty much a collaborative effort among nurses, nutritionists and wound specialists,” says charge nurse and UBT co-lead Toni Leonen. “The nurses are receptive to implementing the various methods we use to prevent pressure ulcers.”
In a span of two years, the new process helped the team reduce the number of bed sores to 0.
“We’ve created this environment where the staff thinks safety and thinks patient comfort,” Kathy Smith, RN, assistant department administrator says. “It’s automatic. They just come in and make sure patients are turned. Nobody has to remind them.”
Coming up with a new process to combat pressure ulcers helped the team build a sense of unity and staff satisfaction, but they also know the work continues.
“Sustaining our success is the biggest challenge because you can revert back to old practices,” Smith says. “You have to keep emphasizing what we’re doing and what the reasons are. Make sure they know you appreciate them so they continue to do well.”
Colorado’s asthma care coordinators discovered that children were refilling their medications at the lowest rate in the region. The group works alongside physicians and staff to provide education and outreach to Kaiser Permanente members with asthma or chronic obstructive pulmonary disease.
Inhaled corticosteroids help control asthma by reducing inflammation and mucus production. Asthmatics who use the meds daily experience fewer attacks, use their emergency medicine less and make fewer visits to the emergency room.
There are some common threads among patients, who don’t refill their prescriptions. These include the costliness of inhalers, the fact some patients are reluctant to take a steroid, and often patients stop medication when they start to feel better.
“It took us a while to identify the most important thing our UBT could do,” said Cindy Lamb, RN, an asthma care coordinator and member of UFCW Local 7. “It was definitely a learning process.”
So, the asthma coordinators decided to improve the refill rate through an outreach program and targeted members ages 5-17. They made phone calls to five members a week who had not refilled their prescriptions in more than four months. As part of the discussion they included talking points about the benefits of inhaled corticosteroids. They used trackers and scoreboards to monitor the outreach and keep everyone informed.
The seven asthma care coordinators were spread throughout the region, so they held weekly phone huddles to share progress and best practices. They highlighted the convenience of the mail order pharmacy, and provided members with prescription refill numbers as well as the telephone number to the pharmacy. This information helped patients refill their medications more promptly.
The team also had communicated regularly with pediatric physicians and other staff by phone, conversations, meetings, and email.
None of it happened overnight, but the team discovered the collaborative effort really helped the process. In all, they reached 1,100 patients.
“Give the process the time it needs,” said Asthma Care Coordination manager Leah Brines. “Resist the temptation to come up with solutions for the team and instead, guide the conversation, and encourage participation and discovery. The team, given the time and confidence, will find the solution.”
When UBT co-leads at Sunnyside Medical Center took a closer look at their patient safety assistant usage, they agreed that reducing the number of hours was a top priority.
The patient safety assistants, also known as PSAs, were certified nursing assistants and provided a key service. They were assigned to sit in a room with a patient who had dementia, was confused or at risk of a fall. They could help if the patient tried to get out of bed, remove their IV lines, or became disoriented or restless.
And patients getting out of bed is not unusual.
Some try to get out of bed because they're bored and restless or they might need to use the bathroom. Restless patients often need a change of scenery, which might mean moving the patient to the nurses' station or to a public area. There might be a need to reduce noise by closing doors at shift change to keep it quiet.
During a five-month stretch, the Sunnyside nursing unit had used 1,550 hours on PSAs. At a cost of $62,000, they wanted to bring those hours down without adversely impacting patient care.
So staff members made it a priority to talk with the patients and families to learn about the patient's interests and hobbies and offer specific activities for patients to do during their stay.
"Using the activity boxes (which contain games, crafts, videos and more) with patients has been a great way to help patients stay busy, and it makes them feel better," according to UBT labor co-chair Glenda Vosberg, RN.
The goal was to reduce PSA usage by 10 percent in four months. Knowing this was going to be a full-team effort, a mandatory in-service was scheduled and the co-leads explained the situation to the rest of the team.
They trained staff on the options to using PSAs. They provided the team with baseline data and information on the financial impact of using PSAs, and had nurses assess patients to determine whether a PSA is needed.
The results were immediate.
In a month, hours dropped from 549 to 32 without any negative impact on patient safety. Within another two months, PSA usage fell to eight hours.
"Staff were given the data and information to help them understand the impact of the situation and get their feedback on alternative options to using a PSA," says Imelda Zapata, department manager and management co-lead.
The team also enlisted the assistance of Susan Woods, the clinical nurse consultant in the hospital.
One of Woods' responsibilities was to provide consultations with patients who were assigned PSAs. She worked with the patient, family and nurse to develop a plan that best fit the needs of the patient.
Kaiser Permanente also invested in several different equipment options, including low beds, which can be put all the way down to the floor, and bed and chair alarms that let nurses know if a patient tries to get up.
The combination of equipment, changes to the environment, and activities for patients allowed the team to keep their patients safe and improve their morale while decreasing the usage of PSAs.
"Often staff is concerned about patient safety when we talk about alternatives to assigning PSAs and may be reluctant to try other options. However, literature (and our local experience) shows that having a PSA in the room does not guarantee the patient won't fall or pull out their IV lines," Woods says. "We've found that reduction of PSA usage has not negatively impacted patient safety, just as the literature suggests."
The Mammography Department at Sunnyside Medical Center was seeing about 370 patients per week, but 25-30 percent of those appointments were running behind schedule.
Appointments ran late because information was missing from the file, additional forms were needed or the wrong test had been ordered. This cost the technologist additional time tracking down information or following up on needed documentation during the patient’s appointment, which had a cascading effect.
The unit-based team (UBT) realized that many of the issues causing delays during appointments could be handled in advance of the patient's arrival. The team came up with the idea of setting time aside every afternoon for a technologist to review the following day's orders.
"Many times patients who are coming in for an appointment are here because something has shown up on a prior screening and their anxiety and stress levels are high,” Cheryl Maize, manager of Mammography, and UBT co-lead says. “By streamlining our appointments and ensuring appointments run on time, we are hoping to allay some of that stress."
Initially, a 3-4 p.m. window was set, but as staff began to test the new process, they learned that starting the work that late in the afternoon was not ideal.
In some cases, they needed to return phone calls or required additional information, and they couldn't get everything done by the end of the day. The team pushed up the pre-work orders to a 1-2 p.m. time slot and the results improved.
In addition, the team implemented a "double-check" system at 4 p.m., so orders were again reviewed to make sure any outstanding items had arrived and everything was ready for the patient's appointment the following day.
The technologist reviewing the orders also would leave notes in the file if there was something the technologist who was seeing the patient needed to know.
Patient experience improved with the new process. Appointments were on time, and technologists were better prepared to work with their patients because the orders had been reviewed in advance.
"The implementation of the screening of orders 24 hours prior to patient arrival has allowed us to maintain our allotted appointment times and has made it easier to accommodate surprises such as late arrivals and walk-ins," Laura Wellnitz, technologist, and UBT labor co-lead says.
Eventually, a technologist was checking orders and printing out appropriate paperwork for diagnostic mammograms one day in advance of the appointments. This eliminated 10-20 minutes per appointment. As a result, most diagnostic appointments were completed in the scheduled 30 minutes, so subsequent appointments started on time.
Other staffers also preferred the new process. They decided to take turns verifying and reviewing orders, which provided a welcome break in the daily routine.
The MRI unit at Kaiser Sunnyside Medical Center had a challenge.
The department was receiving an average of 120 cases each day, but they were able to see only 71. As a result, patients were being referred outside of the Kaiser Permanente system. This drove up referral costs, inconvenienced KP members, and increased dissatisfaction.
In addition, referring patients to outside services posed a delay in getting results back to the ordering doctors. Schedulers who received the request for appointments also had a tough job—when they were not able to accommodate patients within the KP system, they had to make arrangements with outside services, which took additional time.
And finally, the patients didn’t like it.
The feedback from patients to department manager David Barry, was that they didn’t want to have to go elsewhere for services. Patients preferred to have their MRIs performed at the Sunnyside Medical Center.
The team's first step was to increase capacity to see more patients and reduce outside referrals by at least 10 per week within two weeks. To acccomplish this, they reduced the overlap in staffing and changed the schedules of two technologists, increasing their ability to see more patients.
The new staffing schedule, which didn’t infringe on union contracts, came out of a brainstorming session and was supported by staff and physicians.
After the first two technologists adjusted their schedules, a third technologist, seeing the difference it made, offered to adjust his schedule. By the end of one week, about 15 more patients were added to KP’s schedule and not referred to outside services. This resulted in a cost savings of about $7,500 per week, or about $30,000 per month.
"One of the big advantages that we have found is that we have openings for certain appointment types within a day or two, not a week or two," says labor co-lead Heather Thompson.
In addition to the work done in the UBT, a mobile scanner was added to the department. This enabled an additional 11 patients per day to be seen—or about 55 patients per week—for an additional per week savings of $30,000 in outside referral costs.
"There is a downside to that, though,” Thompson says. “Since patients are able to get the appointment so quickly, it seems as though we have a lot more short-notice cancellations and we do not have a wait list to fill them with. That is something that we will need to monitor and try to come up with a solution to."
The folks at the Denver Regional Pharmacy found their unit-based team to be a major improvement over the steering committee it replaced.
Team members found the committee to be unwieldy, and felt it largely bred distrust and miscommunication between union and management.
So, they regrouped.
A major problem they had encountered was the time pharmacy technicians wasted researching prescriptions that weren’t properly "batched." Often missing was the required electronic stamp from a pharmacist that tracks and closes the prescription.
Technicians spent roughly 1-4 hours a day per pharmacy tracking down misbatched prescriptions. The team aimed to cut that time by 50 percent.
"The biggest thing is if you view your situation as a failure you'll never succeed," management co-lead Luanne Petricich says. "When something is not working that's where your opportunity is. Don't be afraid to change something if it's not working."
The team modified the way pharmacists attached their electronic signature. That saved technicians hours of research time and freed them to spend more time with patients. Almost immediately the team saw a drop in the number of prescriptions that needed to be researched.
In the two pharmacies where the team instituted new batching practices, they saw a 75 percent drop in the number of prescriptions requiring research. The new protocol was introduced to 20 pharmacies in the region, and 70 percent of those saw similar gains.
This collaborative effort produced positive results as their projects improved customer service and affordability. The new UBT also gained some hard-earned trust.
Since that success, the regional team has become a model and a sponsor for smaller, pharmacy-specific UBTs launched in the region.
"I like the focus on efficiencies and waste because it ends up translating to a better work environment for employees," Petricich says. "Especially with this project, we found the technicians were doing redundant work that did not provide job satisfaction. So taking that away allowed for more time with patients, which is what many would rather be doing."
Our 2000 National Agreement created the joint LMP Trust Fund. It also created the Performance Sharing Program. It began with these prophetic words:
"This National Agreement was created through an extraordinary collaboration with the input of hundreds of Kaiser Permanente employees at every level. We created this document the way we will work in the future—jointly. The Agreement embodies our collective vision for Kaiser Permanente. The language of this National Agreement cannot begin to fully capture the energy and collective insights of the hundreds of people working long hours to establish this framework. But as work units apply these principles, we trust that their commitment and expertise will make our vision a reality."
The 2018 KP-Alliance National Agreement renews and strengthens the Labor Management Partnership to better serve the needs of our members and patients, the organization and the 49,000 workers represented by the Alliance of Health Care Unions. Alliance union members, their managers, and physicians who work with them should know key provisions of the agreement and what it does to help achieve high-quality, affordable health care while creating a great place to work.
